Over the past month, I have expanded on key drivers impacting I/DD providers observed from the #IDDSummit. One of the biggest shifts for the industry is the transition from fee-for-service (FFS) to value-based reimbursement and alternative models of payment such as managed care (See The I/DD Provider Business Model Must Shift: Why Aren’t You?). Managed care models for I/DD populations are slowly taking hold across the country as stakeholders are growing increasingly comfortable in providing healthcare “value” (See How Can Managed Care Work For The I/DD Population?). The core challenge for I/DD in demonstrating value is how to track and use data that illustrates benefits, validates costs, and determines quality. And finally, does this all improve outcomes for individuals who require life-long care?
For individuals with I/DD, quality isn’t commonly measured in recovery days or improvement rates. Quality in I/DD is unique to the individual and is represented by the evaluation of services being provided and how they are helping the person make progress toward outcomes they value. Achieving this real value for people with I/DD can requires insightful application of behavioral, habilitative, social, and clinical data. And they all must align with payment models to support providers in the delivery system.
Service Delivery Shifts & Challenges with Quality
System transformation in I/DD was catalyzed by the implementation of the Developmental Disabilities and Civil Rights Act and the Americans with Disabilities Act of 1990 that pushed the system to transition from institution-based care to home- and community-based (HCBS) alternatives. This alternative service delivery placed an emphasis on providing individuals with increased access, choice, outcomes, integration, and value.
Through the shift in service delivery, reimbursement for services for the I/DD population did not change. Services have continued to be reimbursed fee-for-service with no ties to outcomes, results, or “value” of the service provided. For a population that requires life-long support, Medicaid expenditures for people with I/DD accounted for 70% of funding for Medicaid HCBS waivers (KFF, 2017). The disassociation between individual needs, service delivery, outcomes, and reimbursement have driven states and payers to look at alternative ways to align the system around quality and outcomes. However, there has been little consensus from the federal government, state Medicaid agencies, and payors on which quality measures and outcomes are most appropriate to monitor the care delivered to this complex population.
Because of their often-complex health needs, individuals with I/DD have unique service utilization patterns that differ significantly from the general and Medicaid-specific populations. This population typically rely on specialty providers to address multiple conditions, access a network of community supports to live and work, and receive social services to supplement quality of life.
This extensive service utilization complicates the ability to develop standard quality measures that are key to driving value-based care and cost savings through managed care. Traditional value-based models capitalize on episodic clinical care and quality measurement is focused around structure and process with clinical- and compliance-based metrics. Standard measures do not include benchmarks for non-traditional health care services, community inclusion, and caregiver support (National Quality Forum, 2016), prevalently used in care for individuals with I/DD in HCBS.
Current Work on Quality Metrics
As more states began managing I/DD populations within Medicaid managed care, stakeholders recognized the need for frameworks and standards that defined quality metrics to monitor care delivery and access to services.
The Council on Quality and Leadership (CQL) created a tool, Personal Outcome Measures®, a 21-indicator tool around five key factors (human security, community, relationships, choices, goals), that assists providers in assessing supports and services to ensure they are person-centered. While this tool is not required or disseminated across all I/DD providers, it is helping providers assign quantitative numbers to qualitative features of supports planning and outcomes.
The National Quality Forum (NQF), under a contract with the Department of Health and Human Services (HHS), extensively studied quality domains, measures, and outcomes for HCBS and frequently used by the IDD community at large (NQF, 2016). While the federal government has endorsed this core set of HCBS quality metrics, they are not required for states nor are they narrowly specific to the complex needs required for individuals with I/DD.
In October 2018, a workgroup of industry stakeholders organized a symposium to develop a common understanding of value-based quality measures for people with I/DD as the industry moves to managed care[1]. A report published by the CQL outlines the findings from this symposium and noted that while traditional clinical and compliance measures for this population are important, measures focused on person-centered choice, social improvements, and adequate supports are increasingly impactful on outcomes for the I/DD population. The workgroup also outlined key requirements for developing quality services for I/DD (See graphic).

New York’s value-based payment arrangement for adults with I/DD outlined six outcomes and measures to assess quality services and drive value (see table below)[2].
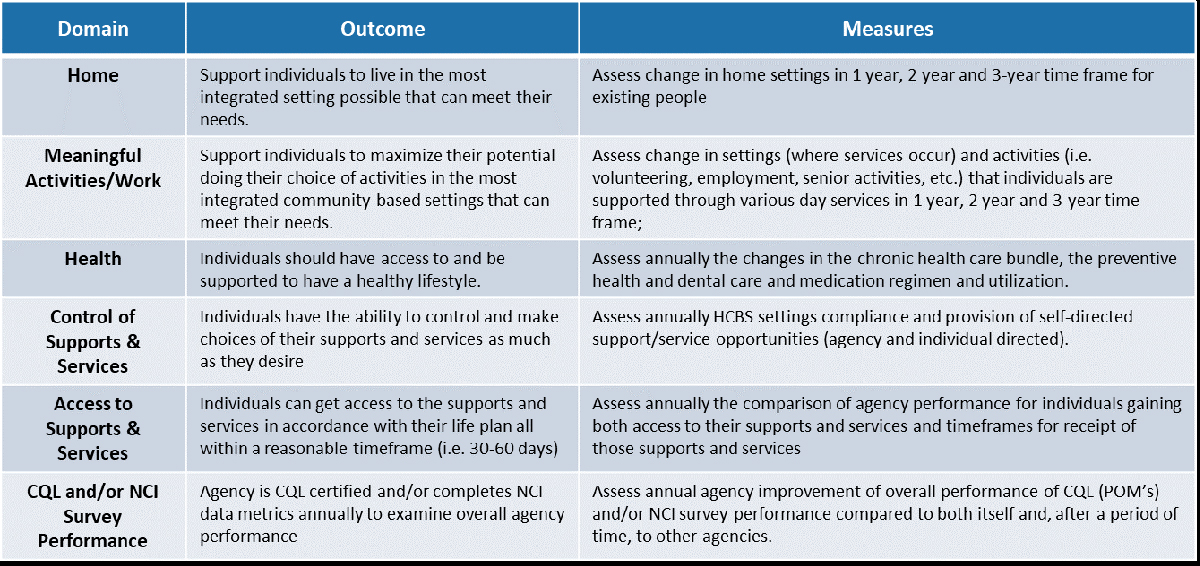
While a lot of work has been done to advance the building of quality frameworks and measures for the I/DD population, there are still a lot of investments to be made in system reform. Inconsistencies between state agencies, support from federal government, and lack of uniform, quantifiable, and reliable data maintained by service providers will continue to present challenges to adopting standard quality metrics. This is a culture change happening across the federal and state bureaucracies.
Provider Considerations with Data and Quality
As the industry moves from utilization to value, I/DD providers will need to be able to generate, understand, and use electronic data to track clinical outcomes, social outcomes, and quality of life outcomes for individuals. Tracking data and integrating quality measures into your leadership discussions, strategy, daily operations, and culture will soon be required.
These performance measures are needed to drive systems change, tie performance to outcomes, allow consumers to make informed choices, and compare the effectiveness of different models of HCBS across the country. Shalock, et al. (2014, 2016, 2018) studied quality measures, sustainability, and improvements in the I/DD system and demonstrated the critical nature of provider buy-in to remain sustainable and to enhance valued outcomes and organization/system performance.
To achieve real value and quality, I/DD organizations should consider redefining the capabilities they will likely need to be effective. This includes determining if your current business model could sustain major shifts in service delivery or payment, implementing tracking tools for consumer feedback, managing data and understanding what it means, investing in technology, and advocating at the state-level for consistency.
[1] Friedman, Carli. (2018). Building The Framework For IDD Quality Measures. 10.13140/RG.2.2.33506.58565.










